Arthur Pienkowski - PharmD et Product Manager Kaduceo
Let’s begin by defining the framework in which the healthcare journey takes place (Figure 1): In France, a user of the healthcare system has a life course, in other words, a set of events that succeed each other, whether they are related to his health or not.
Within this very global framework, a patient has a health journey. The HAS defines it as the result of “the coordinated delivery of health and social benefits to meet the prevention and care needs of individuals, within the framework of controlled expenditures”. The health journey is therefore a concept that includes all care events but also what happens upstream and downstream of them. This concerns both primary and secondary prevention, and medico-social support for health system users

Still according to the HAS, the care path corresponds to: “the right sequence and at the right time of different professional skills directly or indirectly related about healthcare: consultations, technical or biological procedures, medicinal and non-medicinal treatments, management of acute episodes (…)”[2].
The healthcare pathway is therefore a smaller set of the health pathway, focusing only on the healthcare events practiced in connection with an illness. This dimension excludes the notions of prevention and social accompaniment to focus on the steps that take place in the hospital and in ambulatory.
The healthcare journey according to Kaduceo
Kaduceo is an expert company in data analysis about health. For the past 6 years, we have been looking at the healthcare journey from the perspective of the data analysis of the activity from health care institutions:
Time sequence of all care events occurring during medical management.
Figure 2 outlines the characteristics of the care pathway: events (ACE: outpatient procedures and consultations, hospitalizations), duration, flow (intra- and inter-hospital) as well as economic valuation.

Our journey conception begins with the first recording of a patient for a reason in a healthcare facility until the last event of their management.
This approach is based primarily on medical-administrative data from health institutions: the PMSI (Medicalization Program of the Information System). However, other types of data can complement the journey analysis. We are talking about structured databases for data from practitioners' business software, or non-structural databases for medical reports and patients' outgoing letters for example. The scope of a journey and the concepts of start and end are important, especially for cyclical or chronic management. In the example of Medical Assistance to Procreation (in the case of a success), the journey corresponds to all the stages between the first consultation (beginning of the journey) and the delivery (end of the journey). This means that if a couple makes several attempts (IVF, Inseminations) before giving birth, all of these steps will be considered part of the same journey (Figure 3). Despite the possibility of performing several cycles of attempts, the end of the journey remains identified by the “delivery” event. On the other hand, a couple who already had a child through an AMP technique and starting a new attempt, this last one will count as a new journey.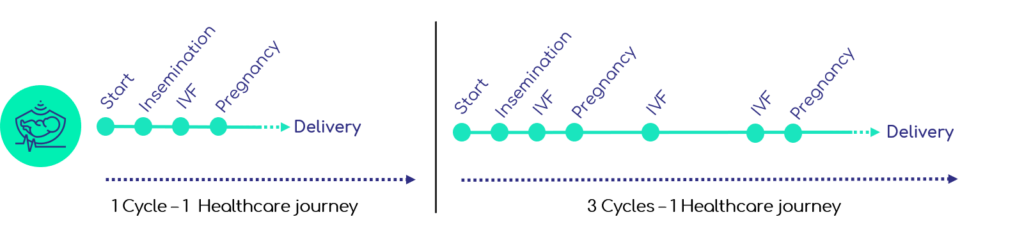
Journey analysis : benefits
When the amount of information to apprehend becomes too important (countless steps, heavy and polypathological patient protocols, etc.) the course analysis brings a global and real vision, a step back on the scale of an entire service (not at the scale of a particular patient). Especially when the volume of activity is high and the care pathway is long and complex. Our approach allows healthcare professionals to gain knowledge and visibility on their practices: identify breaking points, economically value the activity of a service but also analyze relevant monitoring indicators.It is on long and complex paths that data science brings more value to healthcare professionals.The first benefit is therefore medical and operational: by offering an overview of the activity of a service to practitioners to enable the improvement of practices. Since data analysis can also be carried out on an ongoing basis, monitoring of the activity is possible by means of a journey analysis. This management reflects the economic development of a medical unit. Finally, data science applied to the care pathway also supports clinical and scientific research. The Health Data Hub in France is the best example of the growing interest of the medical world in data analysis.
Journey Analysis : Challenges & Stakes
The management of a patient cannot be reduced only when he or she enters a health facility. The “city-hospital” route refers to events related to medical management taking place outside a health facility. This corresponds in particular to:- Procedures and consultations carried out in city medicine (general medicine, specialty medicine, paramedical care, etc.),
- Drug consumption,
- Uses by connected devices for medical purposes (connected medical devices, e-health applications and Digital Therapeutics, etc.).
Bibliography
[1] https://solidarites-sante.gouv.fr/IMG/pdf/2016-01-11_lexique_vf.pdf
[2] https://www.has-sante.fr/upload/docs/application/pdf/2012-05/quest-rep_parcours_de_soins.pdf